Patrick Gilbert PT, DPT, ATC, CSCS
If you have casually perused fitness literature in the past handful of years, you have undoubtedly heard of fascia. If you’ve done a bit more research, you may even know what fascia is and what it is designed to do. If you have taken the time to take a deep dive on it, you probably realize you didn’t know as much as you thought. In fact, many experts are still learning a ton of new information about fascia on a consistent basis. But I digress. Whether you are reading this as a clinician or as a patient, there should be something in here for everyone.
While fascia is incredibly fascinating and important, I want to address dermofascial mobility and restrictions. If you have ever had an old scar or an acute incision from a surgery that doesn’t move like the surrounding skin, you may be dealing with a dermofascial issue. When you break down the word “dermofascial” you are left with two, distinct structures: the dermis (the deeper, thicker portion of the skin), and the fascia (multiple layers of extremely pliable, yet durable tissue that act as a buffer between your skin, adipose (fat) tissue and your muscles).. While this relationship is not frequently highlighted in assessing or treating orthopedic injuries or pain, it can play a key role in resolving impairments related to that pain.
So let’s go over the anatomy and importance of these structures, what happens when the relationship between these tissues goes awry, how to assess and treat impairments of these layers and outline the bigger role this seemingly simple relationship can have on orthopedic issues.
Dermofascial Anatomy
Working your way from superficial (outermost layer) to deep, there are multiple levels or layers of different types of tissue that have unique interactions with each other. When you take the fascial system as a whole, it technically encompasses “adipose tissue, adventitia, neurovascular sheaths, aponeuroses, deep and superficial fasciae, dermis, epineurium, joint capsules, ligaments, membranes, meninges, myofascial expansions, periostea, retinacula, septa, tendons … visceral fasciae, and all the intramuscular and intermuscular connective tissues, including endomysium/perimysium/epimysium”1 Since we don’t have all day to break down every single one of those tissues, we will simplify things.
Fascia is described as “a sheet, or any other dissectible aggregations of connective tissue that forms beneath the skin to attach, enclose, and separate muscles and other internal organs.”1 So at its core, fascia is the layer or layers that separate skin and adipose tissue from muscles and other internal organs. The skin is made up of multiple layers, but for simplicity sake we will break it into two layers; the epidermis, or portion of skin we can visualize from the exterior, and the dermis, the deeper level that is not visible to the human eye. Underneath the skin, we have a (hopefully thin) layer of superficial adipose tissue, which provides some necessary protection and insulation. The next layer is a thin layer of superficial fascia. Beneath the superficial fascial layer is essentially a repeat of the two layers above it, with a layer of fat, then another, thicker layer of deep fascia. Deep to this second fascial layer, sits a layer of hyaluronic acid, designed to assist with lubrication. We will cover this in more detail later. Under all this is the outer covering of the muscle, known as the epimysium and finally the muscle itself. To help picture all these layers together, here is a diagram of this relationship:
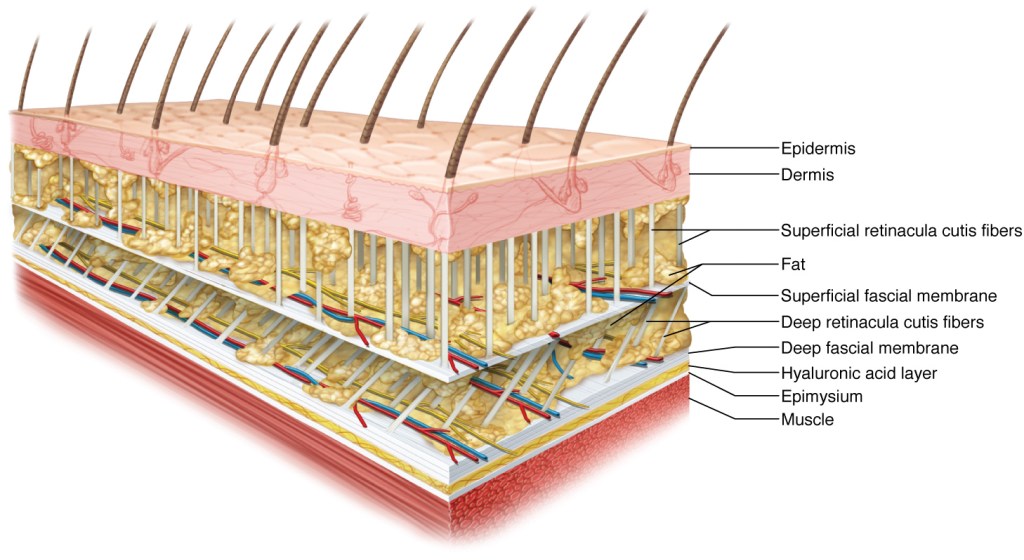
As you can see, there are all sorts of blood vessels and superficial nerves interwoven in these layers, as well as all those other big words I mentioned earlier. For now, we will not worry about those and will just stick to the meat of the discussion.
You might notice that some parts of the body don’t have muscle tissue directly under the skin and have bone much closer to the surface. I’m talking about places like your clavicles, elbows, knees, ankles and parts of your feet, for example. For these bony areas, the layers of skin, subcutaneous fat and fascia need to slide and glide on each other and over the bone rather than muscle. This in itself is not necessarily a problem, but it leaves less “room for error” if inflammation is introduced into the equation.
When Things Go Wrong
When you have irritated tissues, whether it is from acute trauma or a chronic inflammation, the body brings proinflammatory chemicals such as cytokines, macrophages, bradykinin, substance P and proteases1 to that local area to help deal with the injury. The inflammatory materials and fluids that arrive at the site of injury are more viscous (thicker) than normal, non-inflamed fluids and can tend to make those fluids “sticky”. While these chemicals are great for initial, acute injuries and inflammation, they can tend to cause issues if they stick around for too long. When this fluid sits between layers of skin, fat and fascia after the acute stage of inflammation, it creates a difficult environment for these tissues to slide and glide on each other. The result is these separate layers sticking together which does not allow for normal movement between the layers. This is a problem for a couple reasons.
Our tissues and cells stay healthy by performing their duties and being properly nourished. Our bodies actually have specific cells that release hyaluronic acid into connective tissue matrix.2 As I mentioned earlier, and as you can see in the diagram above, hyaluronic acid tends to sit between the deep fascia and the muscle, but it is also found in other areas of the body. It is a substance found in our joints that acts as a fantastic lubricant to keep our joints and other tissues healthy. In a normal, healthy environment, these cells are performing their duty and water is able to penetrate between the layers of tissues ensuring they stay properly hydrated. Sliding, gliding and stretching our skin and fascia allows them to remain healthy and hydrated. A study investigating the role of inflammation on connective tissue found that “stretching of fascial tissues can promote resolution of inflammation”.3 But when inflammation is present and these layers become stuck together, they do not get their normal tissue nutrition and hydration because their surfaces are not interacting with other tissues normally.
Sliding, gliding and stretching our skin and fascia allows them to remain healthy and hydrated
Tweet
Having these layers stuck together can also be a significant source of pain for an individual. As I stated earlier, these tissues are meant to move. They are meant to have intra-tissue (within) stretch and they are meant to have inter-tissue (on others) slide and glide. If they are not allowed to do that, they become stiff and irritated. “Well-ordered fibrils become disorganized under stress, thereby interfering with an orderly sliding motion”4 The less movement that occurs, the stiffer and less nourished they become. The longer they are not allowed to move, the stiffer they become. As you can tell, this can turn into a vicious cycle if kept unchecked and untreated.
Luckily, assessing and treating these dermofascial adhesions can help limit inflammation, irritation and dysfunction. A study that looked at fibrosis and adhesions in rats found that “manual therapy can prevent overuse-induced fibrosis in several fascial tissues”.5 Next, let’s learn how to evaluate and treat these dermofascial mobility restrictions.
***WARNING***
Before you employ this assessment and treatment technique, it is EXTREMELY important that you inform your patient that this technique can be VERY uncomfortable while you are performing it. After explaining the technique, I like to demonstrate it on another part of their body where they are not experiencing pain and where they can see exactly what you are doing. I usually use the soft tissue of the forearm as an example. It will still be uncomfortable, but hopefully not as painful as treating the actual area of pain. Once they confirm their consent you can start assessing and treating their area of pain.
How to Assess Dermofascial Mobility
Assessment of dermofascial adhesions and restrictions is not all that complex. Your aim is to determine what areas are restricted, how limited they are and in what directions are they restricted. Understanding these factors from your assessment will determine your treatment.
Start by examining the area in question. Does it look red or irritated? Is it warmer to the touch than areas around it? Does the skin in that area appear to move normally during active movements by the patient? These can be some of the easiest clues to finding dermofascial restrictions. If it is not so obvious, continue to assess the area manually.
In order to check dermofascial mobility manually, you will take up the skin in your fingers, preferably using the index and thumb of each hand. You want to grasp this skin between these four fingers, then slowly roll the skin between these fingers. The key is to not grab hold of the muscle underneath the area of examination. You want to ensure that you are only holding onto the skin and underlying fat and fascia. Do they move smoothly on each other? Do they feel restricted? It can be helpful to compare this area in question to the contralateral side to check for someone’s “normal” and abnormal.
Once you have determined that there is an area of restriction, you need to find out what specific directions are limited. To determine this, all you need to do is repeat the above step in multiple planes. You want to scan in all planes of movement: horizontal, vertical, diagonal and everywhere in between. Do this to determine if there is one plane of most restriction, if a couple are more restricted than others, or if the entire region appears to have similar restriction.
Treating Dermofascial Adhesions
Like I said earlier, your assessment will drive your treatment. Essentially, your treatment will look the same as how you assessed the area. Like before, you will pick up the skin and fascia between your fingers and roll it over itself. You should start in whichever plane you found to be most restricted and move on to other planes once you have improved the area of most restriction. While you should be fine just using your fingers on some areas of the body, I usually find that using a small piece of Thera-band can help enhance the grip you can get on the skin, which increases efficiency and effectiveness of your treatment. Certain areas of the body without much soft tissue between the skin and underlying bone will be difficult to get a good grip without the Thera-band. You can find Thera-band on both Perform Better and Amazon’s websites.
Much of the time, as soon as you finish treatment to the area, the patient will notice an immediate relief or at least reduction of pain. First, they are so excited that you have stopped inflicting pain that it certainly feels better. But more importantly, by breaking up the adhesions that were present and allowing the layers to move on each other, you will quickly bring nutrients and hydration to the area, creating a rapid sense of relief.
So next time you are working with a patient with a chronically inflamed area with increased pain that doesn’t seem to be getting any better with typical soft tissue mobilization, joint mobilizations or other treatment methods, try testing and treating any dermofascial mobility restrictions that may be present.
References
- Zugel M, Maganaris CN, Wilke J, Jurkat-Rott K, et al. Fascial tissue research in sports medicine: from molecules to tissue adaptation, injury and diagnostics. Br J Sports Med. 2018 August 2:1-9.
- Stecco, C, Fede, C, Macchi, V, Porzionato, A, et al. The fasciacytes: a new cell devoted to fascial gliding regulation. Clin. Anat. 2018 31 (5):667-676.
- Berrueta L, Muskaj I, Olenich S, et al. Stretching impacts inflammation resolution in connective tissue. J Cell Physiol. 2016;231:1621–1627.
- Franchi, M, et al., Tendon and ligament fibrillar crimps give rise to lefthanded helices of collagen fibrils in both planar and helical crimp. J. Anat. 2010 March 216(3):301-309.
- Bove GM, Harris MY, Zhao H, et al. Manual therapy as an effective treatment for fibrosis in a rat model of upper extremity overuse injury. J Neurol Sci.2016;361:168–180.
About the Author – Patrick Gilbert PT, DPT, ATC, CSCS

Patrick is a physical therapist, athletic trainer and personal trainer. He runs Summit Performance and Therapy in Indianapolis, Indiana. He has been training clients of all backgrounds for years and has been a practicing physical therapist since 2016. His training philosophy combines his knowledge of rehabilitation as well as strength and conditioning in order to train clients to achieve great results and avoid injuries in the process. His physical therapy practice focuses on a three-dimensional view and treatment of the body and its many parts. Treatment emphasizes manual techniques and rehabilitative exercises to get patients back to previous activity levels without pain or dysfunction.
For more information about training or rehabilitating with Patrick, contact him at SummitPerformancePT@gmail.com or visit SummitPerformancePT.com
Enter your email below to join Summit Performance and Therapy’s email list!

